The Medicaid redetermination process that concluded in March has created confusion, as many people have lost their coverage, some have been re-enrolled, and others are still awaiting resolution. Since state eligibility reviews began in April, 2023, one in ten Montana residents have lost coverage.
The disarray in Montana stems from Congress’ legislation in 2022 that ended continuous enrollment in Medicaid programs that had been sustained through the Covid-19 emergency. The law, which took effect Mar. 31, 2023, was intended to review eligibility — and to reverse the significant expansion in enrollment that had occurred since 2020.
In Jefferson County, 52% of residents renewed their Medicaid, 39% were disenrolled, and 8% have pending cases, according to June 2024 Federal Public Health Emergency Medicaid Unwind data for Montana.
Jefferson County Commissioner Bob Mullen said that a significant number of older adults with disabilities were affected by the process.
“It wasn’t expected that so many people would lose health coverage,” Mullen said.
Mullen also explained that during COVID-19, the health department allowed extended coverage, but, when redetermination began, the process especially impacted the aging rural population, who struggled to meet qualifying requirements and lost coverage as a result.
“They were disenrolled if they didn’t provide the required paperwork or gave incorrect information,” Mullen added.
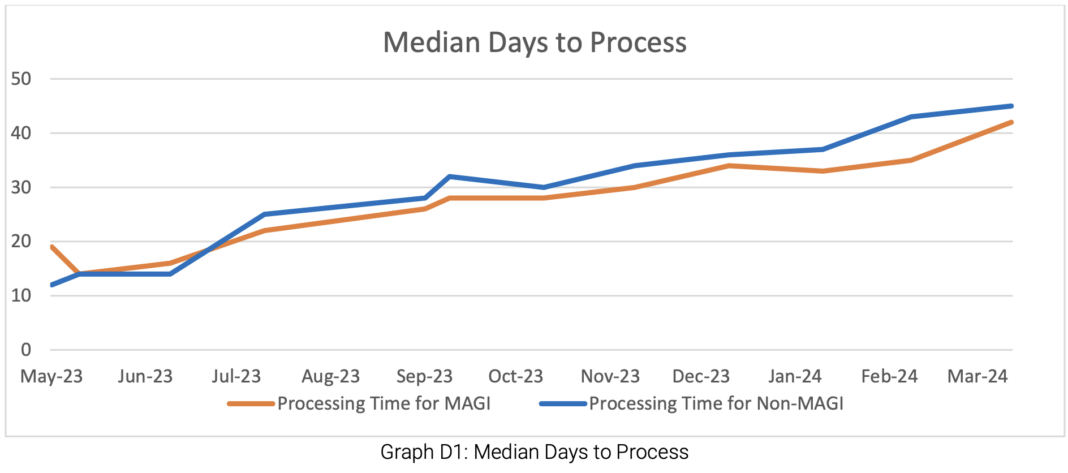
Typically, after the state notifies residents of their Medicaid reevaluation, individuals must complete an online application form. The Medicaid Services office, under the Montana Department of Health and Human Services, then requests additional information, such as proof of income, other insurance coverage, and medical history. This process involves a series of back-and-forth paperwork exchanges, which can leave people confused, often resulting in them providing incorrect information or failing to provide required documents in time.
Sarina Eckman, a Basin resident, began the reevaluation process in November 2023. She didn’t receive any update on her application until February 2024, when the Medicaid office requested her proof of income and specified that, if she didn’t submit it by April 1, she would lose her coverage. She sent in her most recent pay stub but was disenrolled because they required income information from November, not February.
“They never specified that they needed info from the time they started the evaluation,” Eckman said. She lost Medicaid coverage for May and June, going without medication during that time. Eckman recently reapplied and regained her Medicaid coverage.
“It just takes so much time for things to come through the mail, and they don’t have a better way of informing you what’s going on,” Eckman said.
Long-term care facilities are also being impacted, where patients heavily rely on Medicaid support. At Elkhorn Healthcare and Rehabilitation Center (EHRC) in Clancy, between eight and ten patients are undergoing reevaluation.
“I don’t want anyone in the Medicaid office or the claims processors to think we don’t appreciate their efforts—they’re doing the best they can. But there just aren’t enough of them to handle the volume from all the long-term care facilities,” said EHRC administrator Brenda McGaha.
The government continues to provide coverage for previously enrolled patients, but new applications are experiencing delays. According to McGaha, the backlog of existing Medicaid recipients causes delays in reviewing new patient cases, costing the facility around $42,000 per month per patient. Approximately half of the cases currently under review involve new Medicaid applicants.
“We don’t receive any payment until they’re qualified, which can take three to six months. Meanwhile, we continue to provide care, room and board, and medications because that’s our responsibility once they become residents,” McGaha explained.
Due to facility policies, the press is not allowed to speak directly with patients. Gabe Suero, who oversees social services and admissions at EHRC , noted that patients become very stressed upon learning about their Medicaid status.
“When I check in to give them updates, they’re often very worried about whether their care will continue,” Suero said.
The Rocky Mountain Development Council, a private organization managing older adult services in six northwest counties in Montana, including Jefferson County, sent a letter to the Governor’s office on July 19 requesting reforms to the Medicaid disenrollment process for older residents.
The letter called for increased funding for area agencies to address the rising demand for services among older Montanans and proposed professionals-only access to Medicaid information. This would allow agency staff to assist clients more efficiently, avoiding long hold times often experienced by individuals.
Commissioner Mullen, who is also a board member for the Rock Mountain Development Council, emphasized the need for improved communication and new partnerships. “We thought if our clients had a dedicated Medicaid number to call, we could help expedite their application process, especially when issues arise,” said Mullen.