Access to medical care, emergency services and mental health providers emerged as the most urgent concerns of residents in the county Public Health Department’s newly completed Community Health Assessment.
The 2024 assessment is the county’s third such evaluation and the first since the pandemic. It was completed last week, capping a data collection effort that began in spring 2023.
Health departments nationwide are encouraged to conduct these community assessments every three to five years. Jefferson County’s previous assessment was conducted in 2019.Data for the 2024 assessment was gathered through secondary sources, three stakeholder meetings, and 228 responses from residents to a survey comprising 81 questions. The study, funded by the Montana Department of Public Health and Human Services, is intended to inform the county’s Community Health Improvement Plan, a strategic document guiding the development and implementation of policies, projects, and programs that address critical health issues.
“This assessment helps us identify our strengths, challenges, and opportunities for improving health and wellness,” said Pam Hanna, supervisor of Jefferson County Public Health.
The Community Health Assessment utilized various indicators to gauge residents’ health and well-being, including direct healthcare metrics like access to healthcare and infectious diseases, as well as indirect social determinants such as the number of unhoused people.
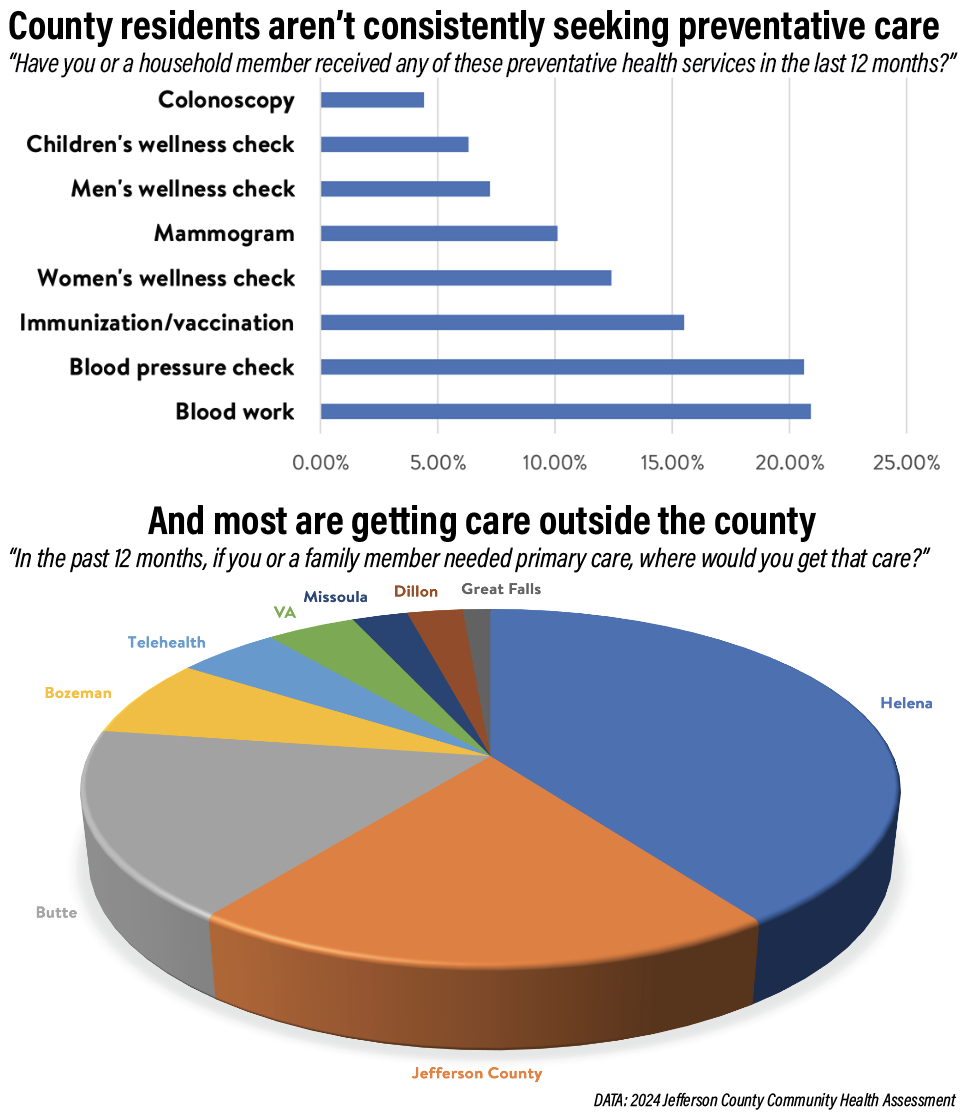
The findings echoed and amplified those of the 2019 assessments. County residents identified a lack of access to quality and affordable medical services as the primary healthcare barrier, according to the assessment. One in ten survey respondents reported not receiving needed healthcare in the past year, while around 50% traveled to Helena for medical services they could not obtain locally.
“We have issues with emergency response and access to medical care throughout the county because of the limits we have what no matter what your income is,” said Hanna. “But people with more resources have the opportunity to have other care.”
The absence of emergency medical services also emerged as a critical issue. The county lacks emergency rooms or urgent care facilities, and one in four respondents reported calling 911 for medical emergencies in 2024.
Mental healthcare remains a focus for the health department. While nearly 75% of survey respondents rated their mental health as good or excellent, the Centers for Disease Control and Prevention’s (CDC) 2022 Division of Population Health Data found that 20.8% of the county’s residents reported experiencing depression. This is slightly higher than the national rate of 19% but below Montana’s average of 22.8%.
In addition, the 2023 National Youth Risk Behavior Survey conducted by the CDC found that one-third of the county’s high school students felt sad or hopeless for at least two consecutive weeks in the past year. Community Health Assessment survey respondents identified cost as the primary barrier to accessing mental health care.
“Mental health is a major concern and was one of the key priorities in our last CHA,” Hanna said. Montana consistently ranks among the five states with the highest suicide rates in the nation. Suicide is the county’s seventh leading cause of death: Between 2018 and 2022, there were 21 suicides, predominantly among males with an average age of 48.3 years.
“Our population is aging. Middle-aged men are becoming a population that we rarely look at with depression and suicide,” Hanna said. “We’re also focusing on our ranching community, where isolation and different stresses are prevalent.”
Substance abuse remains a significant concern for county residents, with the assessment identifying drugs, alcohol, marijuana, and tobacco as key issues. Notably, 27% of adults in the county reported heavy drinking, a rate consistent with the state average but higher than the national average of 19%.
The assessment also included questions about social determinants of health, such as economic stability, quality education, and community context. Rising housing costs emerged as a major concern.
“It might not be within our capability to work on but it definitely impacts people’s health and well-being If they have a safe place to live in” Hanna said.
About 68% of respondents felt there were insufficient low-income housing options in the area, and an increasing unhoused population was also noted as a significant issue.
The Public Health Department will conduct additional stakeholder meetings — intended to help guide the Community Health Improvement Plan beginning July 9 at Volunteer Hall at the county fairgrounds.
“Strategies that we’re going to put in this CHIP are going to be measurable goals so that we can assess whether we are making progress or not,” Hanna said.